
There are pros and cons to every procedure, and surgery is no different.
Here’s what you can expect from a workers’ comp settlement after surgery.
As your doctor is probably quick to remind you, undergoing surgery is a serious matter that requires careful consideration. After all, even a minor procedure can take weeks or even months to recover from.
You may be wondering about the risks associated with surgery, whether you will need to go through physical therapy, or what the long-term complications will be. But if you are recovering from a work injury, you may also be wondering how surgery will affect your claim.
Deciding whether to accept a workers’ comp settlement after surgery or before should not be taken lightly. In this article, we’ll talk about the various factors that may affect your settlement offer and how you can get the most out of your workers’ compensation benefits.
Is Surgery Covered by Workers’ Compensation?
Under Florida law, employees who are injured in the course of their job duties are entitled to receive “medically necessary” treatment and care. This not only includes surgeries, but related hospital stays, rehabilitation, prescriptions, and even lost wages during recovery.

However, it is very likely that the workers’ comp insurance company will not authorize a surgery unless other treatments have failed to produce the desired result. For example, they may request that you visit a chiropractor or physical therapist before authorizing a back surgery.
One main drawback to having surgery through a workers’ comp claim is that you are (in most cases) unable to select your own practitioners. Instead, the workers’ comp insurance company will choose one for you.
However, one major advantage is that all medical treatment you receive through workers’ comp comes at no cost to you—including surgery.
Injured at Work In Florida?
Why Wasn’t My Surgery Authorized?
Surgery—whether under general anesthesia or not—is one of the most complicated medical procedures you can undergo. As a result, they are also one of the most expensive.
If you have a workers’ compensation claim, you don’t have to worry about the medical costs associated with your surgery…but the insurance company does.
They don’t want to spend $25,000 (or even $100,000) if they don’t have to, so even if your authorized treating physician recommends that you have surgery, the insurance company may send you to an Independent Medical Examiner (IME) for a second opinion.
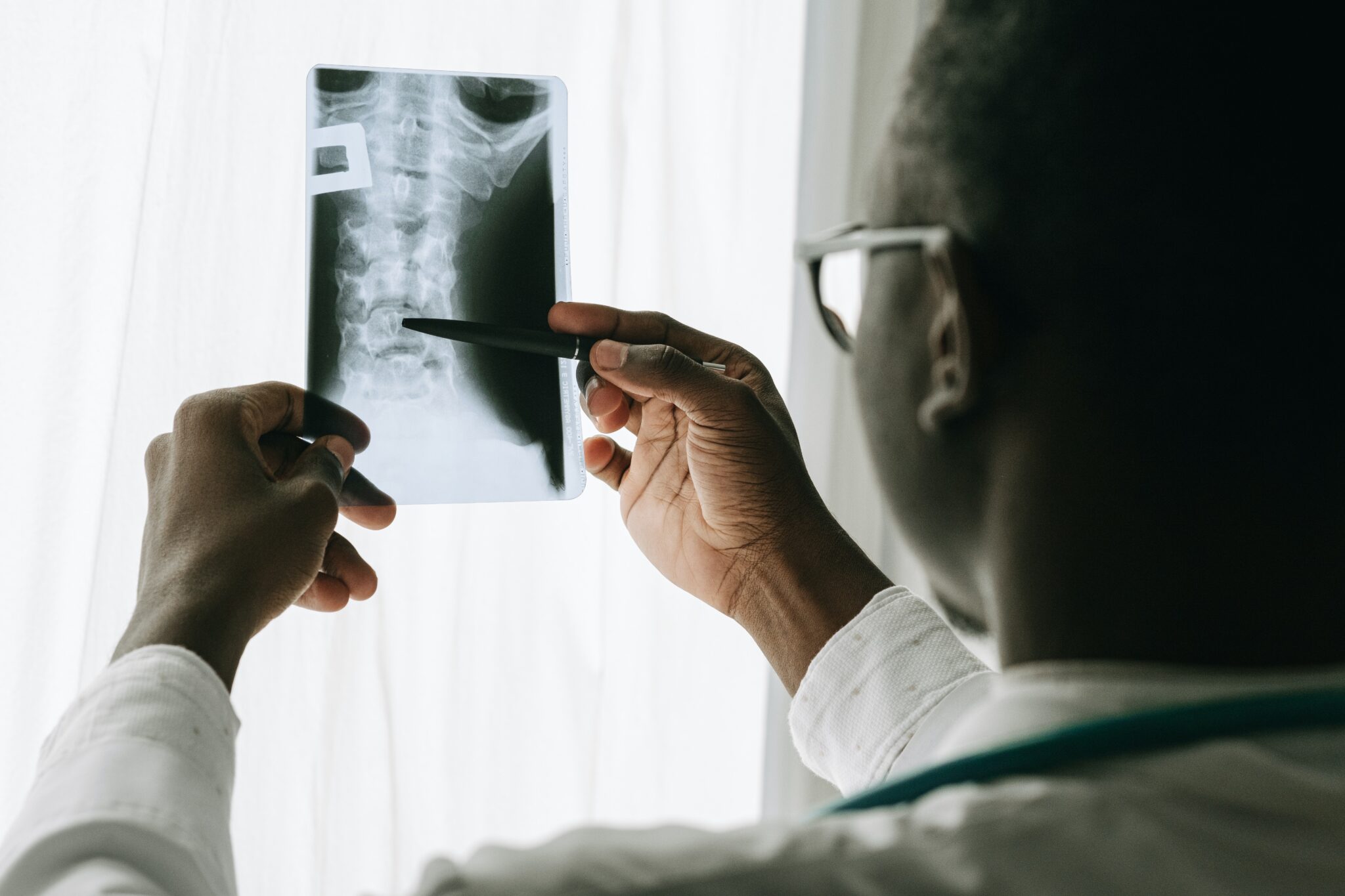
If the IME states that no surgery is necessary, you will need to either follow a different treatment plan or hire a workers’ compensation attorney to litigate your entitlement to the surgery recommended by your authorized treating physician.
This may tempt many injured workers to ask for a settlement so that they can select their own doctors and pursue the care that they deem appropriate. However, this should also be done with caution.
Workers Comp Settlements
In most cases, employees who accept the insurance company’s settlement offer will have to sign a Resignation and Release form that effectively ends their employment and their workers’ comp claim in exchange for a lump sum payment.
This means you will not be able to come back and ask for more money if you run out, even if your condition gets worse.
Settlements are supposed to replace your workers’ comp benefits. If you are accepting a settlement offer so you can get a surgery that the insurance company denied, make sure that the settlement amount is enough to cover any and all future medical care you might need.
How Does Surgery Affect a Workers Comp Settlement?
You don’t always have a choice of whether or not to undergo surgery after a work injury.
For example, if you were involved in an emergency situation, you may have been whisked off to the hospital in an ambulance for a life-saving surgical procedure. Or perhaps the insurance company authorized your treatment.
Does having surgery mean you can expect a hefty settlement?
When determining how much to offer you, insurance companies try to estimate the cost of your future medical bills. The settlement amount is not designed to reimburse you for pain and suffering like a personal injury settlement, but to cover your future medical treatments.
Remember, the insurance company has already covered the cost of the healthcare you have received thus far. The question is what future medical treatment will you need and what will that cost the insurance company.
Get the Most Out of Your Workers Comp Settlement
Regardless of the medical treatment you have received in the past, it is vital that your settlement amount is enough to cover your long-term care needs.
There are a variety of factors to consider, such as your use of medication, routine office visits, whether future surgery is anticipated, other continued health care needs, loss of earning capacity, and permanent impairment rating.
Remember, no medical treatment comes with a guarantee. Whether you’ve had surgery or not, you can’t say with 100% certainty what the future holds for you. Your condition may improve, get worse, or stay the same.
Working with a workers’ comp attorney will give you a much better chance at knowing what your claim is actually worth so that you can get the full amount you’re entitled to receive.
Navigating a workers’ comp claim can be overwhelming, but you shouldn’t have to do it alone. If you have any questions about your settlement amount or your rights as an injured employee, schedule a free consultation with the Law Office of Brian D. Tadros today.

